RADIATION THERAPY
About Radiation Therapy
Radiation therapy, also known as radiotherapy, is a type of cancer treatment Scottsdale, Gilbert, and Phoenix patients can receive through the Phoenix CyberKnife & Radiation Oncology Center. It's one of many available treatments for cancer and can be used as a primary cancer treatment or in combination with surgery, chemotherapy, and/or hormonal and biological therapy.
Those whose cancer is treatable with radiation and qualify for the CyberKnife System will have our team of internationally-recognized radiation oncologists overseeing their care. Our doctors will discuss what treatment options are best for your specific cancer and what role radiation therapy can play in your overall treatment plan.
How Does Radiation Therapy Work?
Radiation therapy uses special equipment to deliver radiation to cancerous cells. Cancerous cells grow and split much faster than normal cells, which makes it important to ensure they are treated quickly and thoroughly. Radiation therapy works to safely and effectively treat cancer and other diseases by damaging these malignant cells. New techniques in radiation therapy allow doctors to accurately target tumors while minimizing the impact on normal surrounding cells. Depending on your cancer, radiation can offer a cure, control the growth of the tumor, or relieve associated symptoms.
Radiation oncologists can administer radiation therapy for a variety of reasons and in a variety of ways. Radiation can be used to cure cancer by:
- Eradicating tumors that have not spread to other parts of your body
- Reducing the risk of cancer returning by killing remaining small amounts of cancer after surgery or chemotherapy
Radiation also may be used in palliative care, or palliation, to slow cancer growth or reduce symptoms caused by growing tumors. Palliative care can be used to shrink life-interfering tumors and relieve pain while reducing the size of the tumor.
To learn more about the role of radiation therapy in your cancer treatment in Scottsdale or the surrounding areas, contact our center today to schedule a consultation with one of our board-certified and internationally-recognized radiation oncologists.
What Are SBRT, SABR, and SRS?
SBRT, SABR, and SRS are the most advanced forms of radiation therapy used in cancer treatment. They stand for stereotactic body radiation therapy, stereotactic ablative radiotherapy, and stereotactic radiosurgery. These specific forms of radiation therapy allow Phoenix CyberKnife and Radiation Oncology Center to deliver high doses of radiation with sub-millimeter precision. SBRT and SABR are often used in the treatment of tumors that are found throughout the body, while SRS is generally when treatment is specific to the brain.
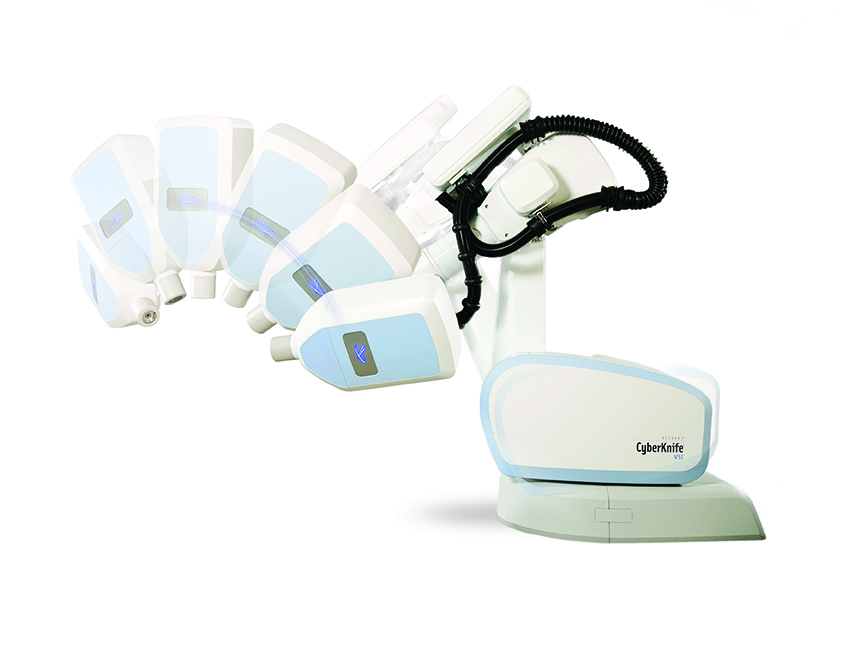
The CyberKnife System features a flexible robotic arm that can adjust to virtually any angle during a radiation therapy session, making it the ideal design for administering SBRT, SABR, and SRS. It also combines real-time image guidance and tumor tracking technology to synchronize and adjust for regular movement that occurs during treatment sessions by the patient’s body as well as the tumor itself. By tracking the tumor and adjusting to it, the CyberKnife System ensures that radiation focuses directly on the tumor and not the healthy tissues or organs.
Because of the advanced imaging and motion tracking technology used by the CyberKnife System, many of the difficulties associated with all other radiation therapy technologies are mitigated. Patients treated with CyberKnife are no longer required to hold their breath, have restrictive frames bolted to their heads, or rely on other techniques designed to stabilize the tumor, compensate for movement, or keep them as still as possible during treatment. Instead, patients who choose SBRT, SABR, or SRS through the CyberKnife System will lie comfortably and breathe freely on the CyberKnife treatment couch during a precise and adaptive radiation therapy session, while the CyberKnife treats the tumor with pinpoint precision.
Other radiation therapy treatments, such as IMRT, IGRT, and Proton Therapy, expose large areas of a patient’s body to smaller doses of radiation. Because of this, conventional treatment often requires 35-45 consecutive days of treatments, taking several months. Because of the high-dosage and extreme precision used by the CyberKnife System, patients who choose SBRT, SABR, or SRS require just one to five sessions and are typically finished within a week of starting treatment. For more information about cancer treatment in Scottsdale, AZ or the surrounding areas, be sure to contact the Phoenix CyberKnife & Radiation Oncology Center today.
External Radiation Therapy Treatments
The goal of radiation therapy is to target tumors with radiation in order to kill the cancer cells while preventing damage to healthy surrounding tissue. There are several ways to do this. Depending on the location, size and type of cancer, you may receive one or a combination of techniques. Your treatment team will help you to decide which approaches are best for your specific diagnosis.
Radiation therapy can be delivered in two ways, externally and internally. During external beam radiation therapy, a machine directs high-energy X-rays at the cancer. Internal radiation therapy, or brachytherapy, involves placing radioactive sources (for example, radioactive seeds) inside your body. In this section, we’ll focus on external beam radiation and the various technologies used to deliver it.
Generally during external beam radiation therapy, a beam of radiation is directed through the skin to destroy the main tumor and any nearby cancer cells. To minimize side effects, the treatments are typically given five days a week, Monday through Friday, for a number of weeks, allowing doctors to get enough radiation into the body to kill the cancer while giving healthy cells time each day to recover.
The radiation beam is usually generated by a machine called a linear accelerator (linac), which is capable of producing high-energy X-rays and electrons that target your cancer. Using high-tech treatment planning software, your treatment team controls the size and shape of the beam, as well as how it is directed at your body, to effectively treat your tumor while sparing the surrounding normal tissue.
There are several types of external beam therapy:
- Three-Dimensional Conformal Radiation Therapy (3D-CRT) - Because tumors come in different shapes and sizes, doctors need to identify the size, shape, and location of the tumor before treating it. 3D-CRT uses computers and special imaging techniques, such as computer-assisted tomography (CT or CAT), magnetic resonance imaging (MRI) and/or positron emission tomography (PET) to create detailed, 3D representations of the tumor and surrounding organs. Your radiation oncologist can then precisely tailor the radiation beams to the size and shape of your tumor with multileaf collimators (see picture, right) or custom-fabricated field shaping blocks. Because the radiation beams are very precisely directed, nearby normal tissue receives less radiation and is able to heal quickly.
- Intensity Modulated Radiation Therapy (IMRT) - IMRT evolved from 3D-CRT and enables your doctor to more precisely target radiation to the shape of the tumor. With IMRT, the radiation beam can be broken up into many smaller “beamlets,” and the intensity of each beamlet can be adjusted individually. Using IMRT, it may be possible to further limit the amount of radiation that is received by healthy tissue near the tumor. In some situations, this also may allow a higher dose of radiation to be delivered to the tumor, potentially increasing the chance of a cure.
- Image-Guided Radiation Therapy (IGRT) - Radiation oncologists use IGRT to help more accurately deliver radiation to tumors. IGRT is designed to compensate for movements of the tumor or patient as a result of breathing or normal bodily functions. IGRT involves conformal radiation treatment guided by imaging, such as CT, ultrasound, or X-rays, taken in the treatment room just before treatment is delivered. All patients first undergo a CT scan as part of the planning process. The imaging information from the CT scan is then transmitted to a computer in the treatment room to allow doctors to compare the earlier image with the images taken just before treatment. During IGRT, doctors compare these images to see if the treatment needs to be adjusted, enabling them to better target the cancer while avoiding nearby healthy tissue. In some cases, doctors will implant a tiny marker in or near the tumor to assist in pinpointing the location of the tumor.
- Stereotactic Radiotherapy - Stereotactic radiotherapy is a technique that allows your radiation oncologist to precisely focus beams of radiation to destroy certain types of tumors. Since the beam is so precise, your radiation oncologist may be able to spare more healthy tissue. This additional precision is achieved by using a very secure immobilization, such as a head frame used in the treatment of brain tumors. Stereotactic radiotherapy is frequently given in a single dose (sometimes called radiosurgery) although certain situations may require more than one dose. In addition to treating some cancers, radiosurgery can also be used to treat malformations in the brain’s blood vessels and certain noncancerous (benign) neurologic conditions. Sometimes a high dose of stereotactic radiotherapy can be focused on a tumor outside the brain and given in a few treatments (typically one to five). This form of treatment is called stereotactic body radiation therapy.
- Proton Beam Therapy - Proton beam therapy uses protons rather than X-rays to treat certain types of cancer and other diseases. The physical characteristics of the proton therapy beam enable doctors to more effectively reduce the radiation dose to nearby healthy tissue. Proton therapy is available at only a few specialized centers in the country.
- Neutron Beam Therapy - Like proton therapy, neutron beam therapy is a specialized form of external beam radiation therapy. It is often used to treat certain tumors that are radioresistant, meaning that they are very difficult to kill using conventional X-ray radiation therapy. Neutrons have a greater biological impact on cells than other types of radiation. Used carefully, this added impact can be an advantage in certain situations. Neutron therapy also is available at only a few specialized centers.
To learn more about radiation therapy and the types of cancer treatment Scottsdale, Phoenix, and Gilbert patients prefer to receive, contact us today.
Brachytherapy
Brachytherapy is the placement of radioactive sources in or just next to a tumor. The word brachytherapy comes from the Greek “brachy” meaning short distance. During brachytherapy, the radioactive sources may be left in place permanently or only temporarily, depending upon your cancer. To position the sources accurately, special catheters or applicators are used.
There are two main types of brachytherapy — intracavitary treatment and interstitial treatment. With intracavitary treatment, the radioactive sources are put into a space near where the tumor is located, such as the cervix, the vagina, or the windpipe. With interstitial treatment, the radioactive sources are put directly into the tissues, such as the prostate.
Sometimes these procedures require anesthesia and a brief stay in the hospital. Patients with permanent implants may have a few restrictions at first and then can quickly return to their normal activities. Temporary implants are left inside of your body for several hours or days. While the sources are in place, you will stay in a private room. Doctors, nurses, and other medical staff will continue to take care of you, but they will take special precautions to limit their exposure to radiation.
Devices called high-dose-rate remote afterloading machines allow radiation oncologists to complete brachytherapy quickly, in about 10 to 20 minutes. Powerful radioactive sources travel through small tubes called catheters to the tumor for the amount of time prescribed by your radiation oncologist. You may be able to go home shortly after the procedure. Depending on the area treated, you may receive several treatments over a number of days or weeks.
Most patients feel little discomfort during brachytherapy. If the radioactive source is held in place with an applicator, you may feel discomfort from the applicator. There are medications that can relieve this discomfort. If you feel weak or queasy from the anesthesia, your radiation oncologist can give you medication to make you feel better.
Depending on the type of brachytherapy you received, you may need to take some precautions after you leave your treatment, particularly if you plan to be around young children or pregnant women. Ask your radiation oncologist or radiation oncology nurse about anything special you should know.
About Radiation Therapy
Radiation therapy, also known as radiotherapy, is one of many available treatments for cancer and can be used as a primary cancer treatment or in combination with surgery, chemotherapy, and/or hormonal and biologic therapy.
Those whose cancer is treatable with radiation and qualify for the CyberKnife System will have our team of internationally-recognized radiation oncologists overseeing their care. Our doctors will discuss what treatment options are best for your specific cancer and what role radiation therapy can play in your overall treatment plan.
How Does Radiation Therapy Work?
Radiation therapy uses special equipment to deliver radiation to cancerous cells. Cancerous cells grow and split much faster than normal cells, which makes it important to ensure they are treated quickly and thoroughly. Radiation therapy works to safely and effectively treat cancer and other diseases by damaging these malignant cells. New techniques in radiation therapy allow doctors to accurately target tumors, while minimizing the impact on normal surrounding cells. Depending on your cancer, radiation can offer a cure, control the growth of the tumor, or relieve associated symptoms.
Radiation oncologists can administer radiation therapy for a variety of reasons and in a variety of ways. Radiation can be used to cure cancer by:
- Eradicating tumors that have not spread to other parts of your body.
- Reducing the risk of cancer returning by killing remaining small amounts of cancer after surgery or chemotherapy.
Radiation also may be used in palliative care, or palliation, to slow cancer growth or reduce symptoms caused by growing tumors. Palliative care can be used to shrink life interfering tumors and relieve pain while reducing the size of the tumor.
To learn more about the role of radiation therapy in your cancer treatment, contact our center today to schedule a consultation with one of our board-certified and internationally-recognized radiation oncologists.
What is SBRT, SABR, and SRS?
SBRT, SABR, and SRS are the most advanced forms of radiation therapy used in cancer treatment. They stand for stereotactic body radiation therapy, stereotactic ablative radiotherapy, and stereotactic radiosurgery. These specific forms of radiation therapy allow Phoenix CyberKnife and Radiation Oncology Center to deliver high doses of radiation with sub-millimeter precision. SBRT and SABR are often used in the treatment of tumors that are found throughout the body, while SRS is generally when treatment is specific to the brain.

The CyberKnife System features a flexible robotic arm that can adjust to virtually any angle during a radiation therapy session, making it the ideal design for administering SBRT, SABR, and SRS. It also combines real-time image guidance and tumor tracking technology to synchronize and adjust for regular movement that occurs during a treatment sessions by the patient’s body as well as the tumor itself. By tracking the tumor and adjusting to it, the CyberKnife System ensures that radiation focuses directly on the tumor and not the healthy tissues or organs.
Because of the advanced imaging and motion tracking technology used by the CyberKnife System, many of the difficulties associated with all other radiation therapy technologies are mitigated. Patients treated with CyberKnife are no longer required to hold their breath, have restrictive frames bolted to their heads, or rely on other techniques designed to stabilize the tumor, compensate for movement, or keep them as still as possible during treatment. Instead, patients who choose SBRT, SABR, or SRS through the CyberKnife System will lie comfortably and breathe freely on the CyberKnife treatment couch during a precise and adaptive radiation therapy session, while the CyberKnife treats the tumor with pin-point precision.
Other radiation therapy treatments, such as IMRT, IGRT, and Proton Therapy expose large areas of a patient’s body to smaller doses of radiation. Because of this, conventional treatment often requires 35-45 consecutive days of treatments, taking several months. Because of the high-dosage and extreme precision used by the CyberKnife System, patients who choose SBRT, SABR, or SRS require just one to five sessions and are typically finished within a week of starting treatment.
External Radiation Therapy Treatments
The goal of radiation therapy is to target tumors with radiation in order to kill the cancer cells while preventing damage to healthy surrounding tissue. There are several ways to do this. Depending on the location, size and type of cancer, you may receive one or a combination of techniques. Your treatment team will help you to decide which approaches are best for your specific diagnosis.
Radiation therapy can be delivered in two ways, externally and internally. During external beam radiation therapy, a machine directs high-energy X-rays at the cancer. Internal radiation therapy, or brachytherapy, involves placing radioactive sources (for example, radioactive seeds) inside your body. In this section, we’ll focus on external beam radiation and the various technologies used to deliver it.
Generally during external beam radiation therapy, a beam of radiation is directed through the skin to destroy the main tumor and any nearby cancer cells. To minimize side effects, the treatments are typically given five days a week, Monday through Friday, for a number of weeks, allowing doctors to get enough radiation into the body to kill the cancer while giving healthy cells time each day to recover.
The radiation beam is usually generated by a machine called a linear accelerator (linac), which is capable of producing high-energy X-rays and electrons that target your cancer. Using high-tech treatment planning software, your treatment team controls the size and shape of the beam, as well as how it is directed at your body, to effectively treat your tumor while sparing the surrounding normal tissue.
There are several types of external beam therapy:
- Three-Dimensional Conformal Radiation Therapy (3D-CRT) - Because tumors come in different shapes and sizes, doctors need to identify the size, shape and location of the tumor before treating it. 3D-CRT uses computers and special imaging techniques, such as computer assisted tomography (CT or CAT), magnetic resonance imaging (MRI) and/or positron emission tomography (PET) to create detailed, 3D representations of the tumor and surrounding organs. Your radiation oncologist can then precisely tailor the radiation beams to the size and shape of your tumor with multileaf collimators (see picture, right) or custom fabricated field shaping blocks. Because the radiation beams are very precisely directed, nearby normal tissue receives less radiation and is able to heal quickly.
- Intensity Modulated Radiation Therapy (IMRT) - IMRT evolved from 3D-CRT and enables your doctor to more precisely target radiation to the shape of the tumor. With IMRT, the radiation beam can be broken up into many smaller “beamlets,” and the intensity of each beamlet can be adjusted individually. Using IMRT, it may be possible to further limit the amount of radiation that is received by healthy tissue near the tumor. In some situations, this also may allow a higher dose of radiation to be delivered to the tumor, potentially increasing the chance of a cure.
- Image Guided Radiation Therapy (IGRT) - Radiation oncologists use IGRT to help more accurately deliver radiation to tumors. IGRT is designed to compensate for movements of the tumor or patient as a result of breathing or normal bodily functions. IGRT involves conformal radiation treatment guided by imaging, such as CT, ultrasound or X-rays, taken in the treatment room just before treatment is delivered. All patients first undergo a CT scan as part of the planning process. The imaging information from the CT scan is then transmitted to a computer in the treatment room to allow doctors to compare the earlier image with the images taken just before treatment. During IGRT, doctors compare these images to see if the treatment needs to be adjusted, enabling them to better target the cancer while avoiding nearby healthy tissue. In some cases, doctors will implant a tiny marker in or near the tumor to assist in pinpointing the location of the tumor.
- Stereotactic Radiotherapy - Stereotactic radiotherapy is a technique that allows your radiation oncologist to precisely focus beams of radiation to destroy certain types of tumors. Since the beam is so precise, your radiation oncologist may be able to spare more healthy tissue. This additional precision is achieved by using a very secure immobilization, such as a head frame used in the treatment of brain tumors. Stereotactic radiotherapy is frequently given in a single dose (sometimes called radiosurgery) although certain situations may require more than one dose. In addition to treating some cancers, radiosurgery can also be used to treat malformations in the brain’s blood vessels and certain noncancerous (benign) neurologic conditions. Sometimes a high dose of stereotactic radiotherapy can be focused upon a tumor outside the brain and given in a few treatments (typically one to five). This form of treatment is called stereotactic body radiation therapy.
- Proton Beam Therapy - Proton beam therapy uses protons rather than X-rays to treat certain types of cancer and other diseases. The physical characteristics of the proton therapy beam enables doctors to more effectively reduce the radiation dose to nearby healthy tissue. Proton therapy is available at only a few specialized centers in the country.
- Neutron Beam Therapy - Like proton therapy, neutron beam therapy is a specialized form of external beam radiation therapy. It is often used to treat certain tumors that are radioresistant, meaning that they are very difficult to kill using conventional X-ray radiation therapy. Neutrons have a greater biologic impact on cells than other types of radiation. Used carefully, this added impact can be an advantage in certain situations. Neutron therapy also is available at only a few specialized centers.
Brachytherapy
Brachytherapy is the placement of radioactive sources in or just next to a tumor. The word brachytherapy comes from the Greek “brachy” meaning short distance. During brachytherapy, the radioactive sources may be left in place permanently or only temporarily, depending upon your cancer. To position the sources accurately, special catheters or applicators are used.
There are two main types of brachytherapy — intracavitary treatment and interstitial treatment. With intracavitary treatment, the radioactive sources are put into a space near where the tumor is located, such as the cervix, the vagina or the windpipe. With interstitial treatment, the radioactive sources are put directly into the tissues, such as the prostate.
Sometimes these procedures require anesthesia and a brief stay in the hospital. Patients with permanent implants may have a few restrictions at first and then can quickly return to their normal activities. Temporary implants are left inside of your body for several hours or days. While the sources are in place, you will stay in a private room. Doctors, nurses and other medical staff will continue to take care of you, but they will take special precautions to limit their exposure to radiation.
Devices called high-dose-rate remote afterloading machines allow radiation oncologists to complete brachytherapy quickly, in about 10 to 20 minutes. Powerful radioactive sources travel through small tubes called catheters to the tumor for the amount of time prescribed by your radiation oncologist. You may be able to go home shortly after the procedure. Depending on the area treated, you may receive several treatments over a number of days or weeks.
Most patients feel little discomfort during brachytherapy. If the radioactive source is held in place with an applicator, you may feel discomfort from the applicator. There are medications that can relieve this discomfort. If you feel weak or queasy from the anesthesia, your radiation oncologist can give you medication to make you feel better.
Depending on the type of brachytherapy you received, you may need to take some precautions after you leave your treatment, particularly if you plan to be around young children or pregnant women. Ask your radiation oncologist or radiation oncology nurse about anything special you should know.
